askmyGP joins Evergreen Life for a huge step forward in patient-led healthcare
Evergreen Life is proud to announce the acquisition of Salvie Ltd, the creators of online consultation and workflow system, askmyGP. The two will now work together to help GPs, Clinical Commissioning Groups, Primary Care Networks, and health boards to manage caseloads and strengthen relationships with patients.
The acquisition presents a valuable opportunity for both companies to harness the others’ technical expertise and software experience. The two combined will allow for a wider scope of operations in primary care and better patient engagement, helping both companies progress towards their shared vision of facilitating better access to healthcare for individuals.
What is askmyGP?
askmyGP allows patients and carers to outline their issue quickly and simply in their own words. This enables busy surgery teams to efficiently triage requests, prioritise patients appropriately and minimise wait times. Founded by Harry Longman, askmyGP has been supporting GPs in managing their workload since 2011.
askmyGP serves GP practices with over two million patients and now expands Evergreen Life’s primary care services to include online consultations, including secure video and messaging. Individuals can be assured they always receive medical advice from trained NHS professionals via easily accessible digital channels, further developing the trust between patient and clinician.
What is Evergreen Life?
Established in 2014 in Manchester by former clinical pharmacist, Stephen Critchlow, the Evergreen Life app provides a handy way for people to access their medical records electronically and manage their healthcare online – users can request help or order a repeat prescription. The app also offers Wellness Check functionality to help people better understand their health by taking clinically-reviewed questionnaires to improve various aspects of their wellbeing such as sleep, fitness, diet and happiness.
“We believe in putting the individual at the heart of their own healthcare, so people can be empowered to get the health and wellbeing they want and get access to support when they need it. askmyGP is leading the way in person-centred solutions by making it easier for patients to talk to their own doctor and help GPs to prioritise and deliver care through message, phone and video. By working together and through the new Evergreen Connect platform, we can join up more areas of the health and care system as part of our mission to deliver People Powered Health,” said Mark Hindle, COO of Evergreen Life.
“We are joining a company well-established in the healthcare technology industry and which complements our work in being able to offer more to patients, GPs and other healthcare providers. askmyGP enables over 200 GP practices around the UK to manage their workflow and respond to patient demand with outstanding service, resolving 79% of requests on the same day,” said Harry Longman, CEO and founder of askmyGP.
Patients will benefit from a wider range of services and communications with their GP, and through the Evergreen Life app will be able to take better control of their own health. Providers will benefit initially from integration with clinical systems across the full range of patient facing services and better communications with patients through the app. As our products and services develop, they also gain from people taking control of their health, wellbeing and medical records.”
For more information about Evergreen Life visit: https://www.evergreen-life.co.uk/
ENDS
- Published in News
Who chooses how a patient sees their GP?
It’s a hotly contested topic. Data on what happens might help.
England’s Health Minister Sajid Javid said this week “Where patients have a desire to be seen face-to-face, and this has been an issue recently, I think that choice should be respected.”
Many would agree from both the patient and GP perspective, and respect should be at the heart of the relationship. The rub is when respecting choice becomes compulsory, and here the GP profession is loudly objecting. The GMS contract is silent on the mode by which patients are helped, the professional discretion of the practitioner being paramount.
So how might data inform the debate?
In the previous blog we looked at choices made by patients on the mode of response they would prefer, from the weekly 140,000 askmyGP requests. We can then track what happens to each one, as the GP or other practice staff member records the actual mode by which the request is completed.
The Sankey chart is an analytical joy, named after Captain Sankey in 1898 for his steam engines, earlier made famous for illustrating Napoleon’s 1812 Russian campaign. Adaptable to the flow between stages of any process, it brings instant illumination. It’s exactly what we need here to show the flow between patient preference and outcome with the GP or other staff.
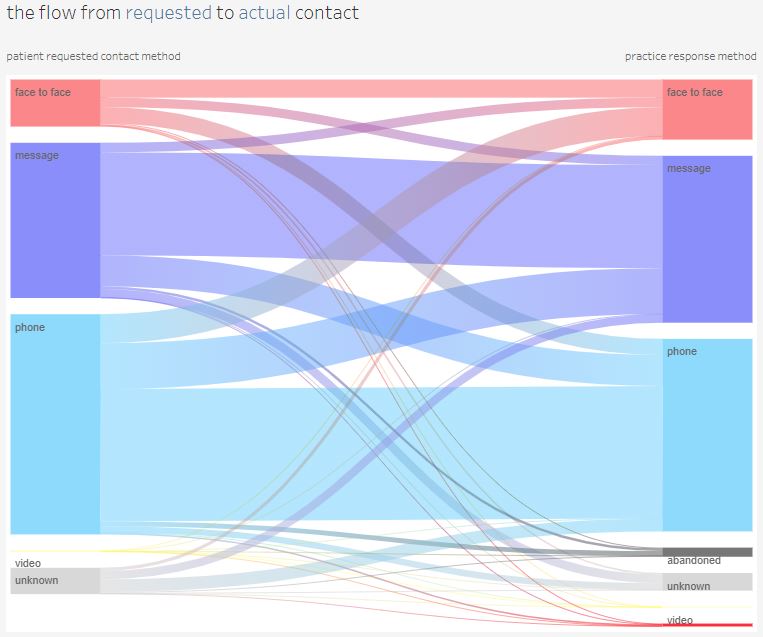
The key points on face to face consultations:
– more patients had a f2f than asked for one
– only one third who asked for f2f got one
– most of those seen f2f had asked for telephone, and many only for a message response
What if patient preference ruled every time?
The data suggests the proportion of face to face would go down, and a number of patients would not be seen, because they asked for a telephone or message response. Of course, we can’t be sure what would have happened in an imagined scenario.
What is clear from the data that is that GPs are making the clinical choice to ask patients to come in even if they don’t want to.
As a patient, isn’t that exactly what you would want?
As a GP, isn’t that the discretion your work requires?
Harry Longman
Source: askmyGP live analytics
- Published in Evidence
How do patients want help from their GP? The data.
We ask patients 140,000 times each week. The answer may surprise you.
This week has provided one of those occasions when national debate is focussed on an area where we collect relevant data, and as all doctors know, effective treatment requires sound diagnosis.
A patient sending a request through askmyGP, whether online (67%) or phoning the practice, is asked for their preferred response. We’ve asked for three years and were surprised that, pre-pandemic, only 30% asked for face to face. Perhaps more surprising is that the most recent weeks show the same data at 10% asking for face to face (chart on the left, red for face to face). On the right, actual response, shows 13% are resolved face to face. GPs are seeing more patients than ask to be seen.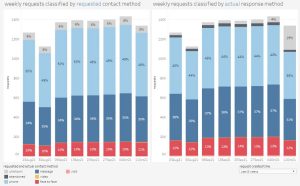
The gravitational forces on general practice underline the pressures:
– 4% growth in population over 5 years, and increasingly elderly at that.
– 5% drop in GP fte numbers, coping with increased demands post-pandemic as secondary care delays leave patients in need for longer.
Should there be more pressure to see patients face to face?
We have never expressed a view on the “right” proportion of face to face, as the clinical judgment of the GP for every patient and need is paramount. All we can do is reflect the data, and try to make the process of collecting and responding to patient requests as easy and flexible as possible, managing the whole workflow as one. GPs tell us all the time that is what they value most.
Sajid Javid said yesterday “My only target is choice” and if there’s one thing we can agree on, it’s that. Arbitrary numbers, with penalties for deviation, cannot be consistent with clinical choice or with boosting morale.
It is clear that going back to a 2019 GP service model won’t work and radical change is needed. A little extra cash won’t fix it, and more GPs will take years to train. Yet we know, from helping hundreds of practices, that right now, GPs with freedom and flexibility are providing a superb service to their patients, and keeping their trust.
Mr Javid, please trust and support GPs to do the right thing.
Harry Longman
Chief Executive
Wigan Borough CCG improves patient experience and builds capacity
How an online total triage solution improved patient experience and is helping to increase capacity – Jonathan Kerry, Associate Director of Primary Care explains
NHS Wigan Borough CCG has 58 GP practices varying in size from small to large. One of its larger practices has a patient list of 17,500 patients, while the average is around 5,000. Until the COVID-19 pandemic hit, just a handful had made the switch to digital working and total triage solutions. However in March 2020, when the doors shut, most practices faced a rapid implementation of digital systems to ensure GPs could continue to provide a service to their patients. The CCG recommended the askmyGP total triage solution and throughout the primary care networks (PCNs) practices started working together to learn from and support one another. Since then, the practices of Wigan have managed over one million patient requests via the askmyGP system, providing an extensive and robust dataset with which to improve ways of working. As well as improving the patient experience, data from askmyGP provides actionable insight, highlighting ways in which workflows can be improved by creating capacity and ensuring all patients are seen by the right person at the right time, while also helping to relieve the significant pressures currently being felt by GPs.
Standardisation leads to greater collaboration and new ways of working
When the COVID-19 pandemic took hold, the shift to digital had already been specified by the CCG within its primary care contracts. Many practices were behind schedule, but consideration also had to be given to how a total triage system could take healthcare forward. The CCG wanted to look beyond the pandemic to improving capacity and access in the future rather than just being a bolt on option giving patients an additional way to book an appointment.
Jonathan Kerry is Associate Director of Primary Care for NHS Wigan CCG. He says the PCNs supported this approach while also encouraging as much standardisation as possible across the system. He says: “If you can standardise at PCN level it makes it easier for practices during a challenging time. Even if it’s just sharing staff and providing resilience these are still worthwhile benefits.”
The push for standardisation was successful. Currently there are 43 practices out of 58 using askmyGP, giving 24/7 access to GP services. Jonathan says: “It helps to identify who is in most need, those who might need face to face or a different type of consultation method.
The PCNs supported standardisation between practices by creating working group forums, aiding learning about how askmyGP can be used to increase efficiency and make positive change. Having already worked together in the form of neighbourhood clusters since 2013, there were ready-made working groups for many clinical leads such as practice managers and nurses as well as patient forums.
Bringing everyone together to discuss any challenges or concerns meant that it was possible to take insight from askmyGP and create an action plan for change. Key to the success of the system is being able to offer core GP services and 24/7 access, but also helping patients to understand if other services can provide the help they need.
A recent snapshot survey by Pulse has revealed that waiting times for GP services across the UK came down during the pandemic as a result of online triaging and remote consultation.
The findings from May reveal the average waiting time for a non-urgent in-person appointment following triage is down to 8.7 days, while the average wait for a phone or video consultation is 7.4 days. GP practices in Wigan using askmyGP have achieved a median waiting time of just 217 minutes.
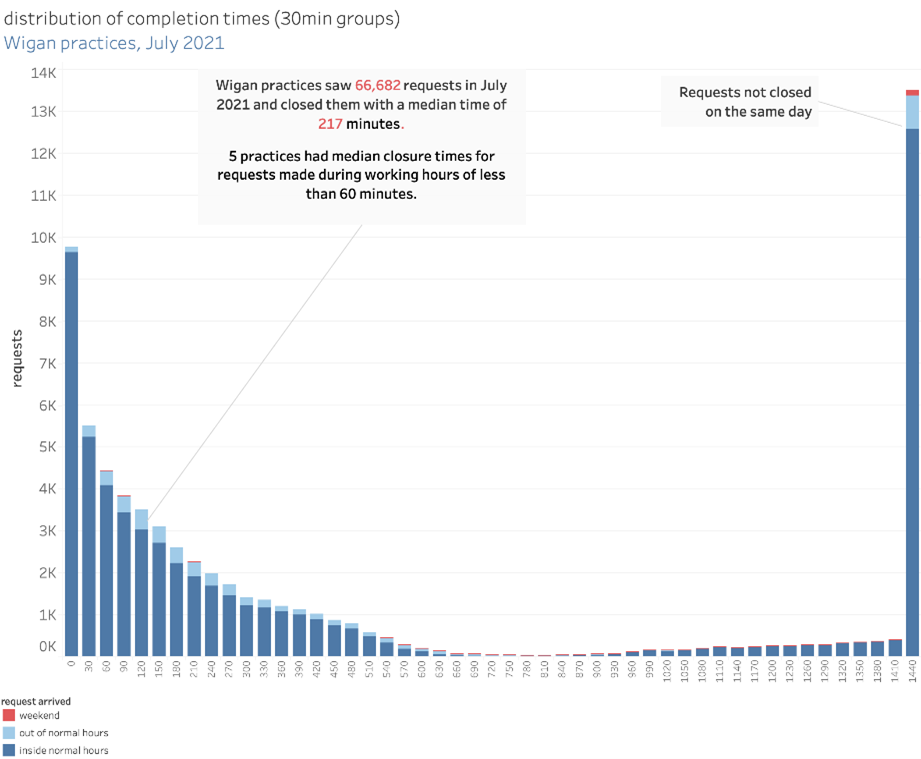
However demand has risen, and GPs are doing more consultations than ever, creating significant pressures. By having several surgeries operating from the same system, it can mean sharing responsibilities rather than having all those surgeries simply replicating the way they work.
For example the PCNs in Wigan CCG have collaborated with a First Contact Physio initiative, which aids triage, helping to signpost the patient to the most appropriate person, rather than automatically seeing the GP as the first port of call.
Jonathan says: “It may not be a physio, but a social prescriber or community link worker. We just need to be able to get patients to the person who can help them and support them best. We can use the technology to underpin that and support them.”
“This is a good example of how to start, it was a rapid implementation to help practices during the COVID-19 pandemic, but the way that we are using First Contact Physios shows the potential and longevity of that way of working.
Expanding capacity and creating new ways of working
The introduction of online triage has been a broadly positive move for patients.
Feedback from the Friends and Family Test has been significantly higher than it has ever been. Over the last 12 months ratings have ranged from 75 to 90 per cent of people saying the service has been better or excellent compared to previous visits. “From a patient point of view, generally there is real positivity for it,” says Jonathan.
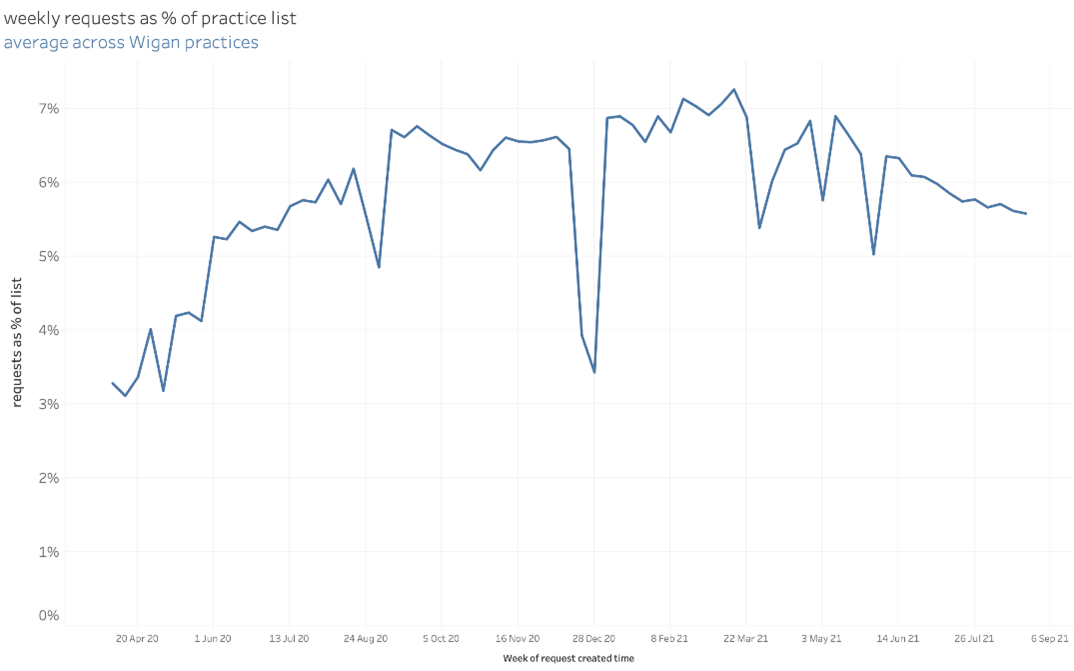
There are also encouraging signs from the National GP Patient Survey, taken in the first three months of 2021, which has shown the CCG area to be higher than average in its use of digital and around access to GPs.
However, Jonathan acknowledges that, while online triaging can be extremely positive for many, there is the potential that it can exacerbate inequalities. He says: “This is something that is always going to be there, so we have to keep working at it and making sure we are doing the right thing.”
With askmyGP, patients can choose their method of contact. If they’re not online, the system is set up to ensure they get the same service should they need to phone the surgery or go in person. No-one should ever be forced to use the online system if they don’t want to.
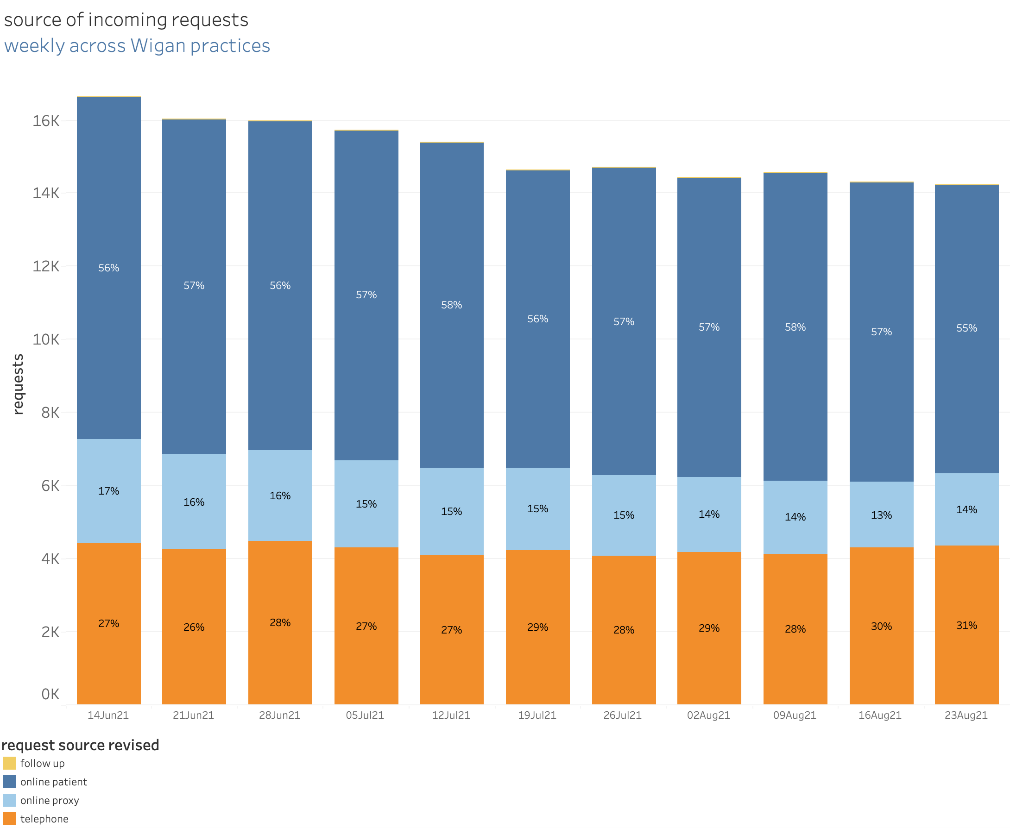
The CCG is currently carrying out market research looking in more detail at the expectations of patients. Speaking to around 3,000 people, the CCG will formulate patient models to help them better understand patient need and see how they can evolve over the next decade.
Regular data can help surgeries hold a mirror up to the way they work
askmyGP generates data daily that can help practices track how they are working and focus on where change needs to be made. The data shows how the system is being used and the mechanisms which patients choose to make contact along with the reasons why.
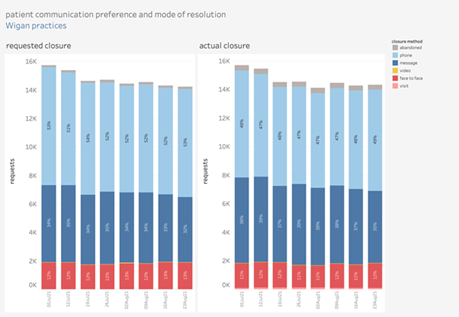
Jonathan says: “Data is critical to enable us to hold that mirror up to see if we can do things more effectively. It gives us a much better understanding of what is going on, for example, have we really had 50,000 patient contacts in the last two weeks or is it 40,000 with the other 10,000 being patients trying to make follow up appointments? Are we creating demand because of the way we are working?”
Analysing data at that level can help surgeries to understand high intensity users, looking at those who have complex needs and seeing how they GPs can support them better.
By building collectively on an effective programme of change, supported by detailed data for improvement, the practices of Wigan are set to remain leaders in patient access to general practice.
- Published in Case studies
GPAD data submissions to NHS England
This note is to update users on data submissions to NHS England for activity reporting.
You may know that practices are required to submit activity data from 30 June 2021 as outlined on their website here.
Many practices made representations that this would create extra work for no benefit, as many patient requests are completed with no need for an “appointment” record.
We have seen a copy of a post on the forum “FutureNHS” by “Digital First Primary Care”
We are raising this with system suppliers with the aim to gather that data directly from them. If a Practice has started / or is happy to map across both systems, this would ultimately create a better reporting data and Practices can continue to do this.
However, if this is not currently being recorded in the GP Clinical system appointment book, the current advice is not to double record in the GP Clinical System appointment book due to the extra burden on Practices.
When the data is published it will include a caveat highlighting that the GP appointment book is not the only tool which captures appointments and for those appointments captured elsewhere we have not got the means of capturing that data.
We have requested an official communication to this effect but have had no reply so far.
The message seems to be a positive one, there is no need to double enter and no further action is required.
We have enabled a feature in askmyGP which allows you to specify a role, compatible with GPAD reporting, for each staff member. We suggest you state a suitable role from the drop down list in the staff record, which is done only once and would take a few minutes for the whole practice. Any reporting needs should then automatically be covered.
- Published in News
How do access hours affect online GP demand?
Demand in general practice is high for the time of year, not just in the media but in the data. It may result from a combination of changes coming out of lockdown, delays in secondary care or easier access, but we don’t have convincing evidence of which is most significant.
The question of what to do about it can’t be separated from the cause, as a wrong diagnosis and resulting wrong solution may make the situation worse. Some have speculated that easier access online is driving up demand, which sounds logical although we saw no evidence of that pre-covid. Nevertheless, if better access has uncovered unmet need that was there all along, what should be done?
One suggestion is to reduce the hours in which online access is available, and Steve Black has taken a look at the outcomes in terms of total demand as a % of list size, since the start of 2021. In the first example, online is available 24/7, although patients are told if they are out of hours to expect a reply on the next working day. Grey bars represent availability, and the red line shows total demand.
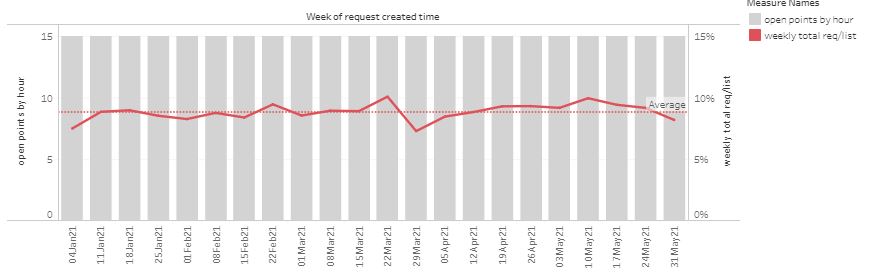
“Open point” is a score based on the period when patient requests can be submitted, weighted towards normal contracted hours. The red line is total demand (online and telephone requests) as a % of list size, per week.
In the following example, opening hours were cut in response to perceived high demand.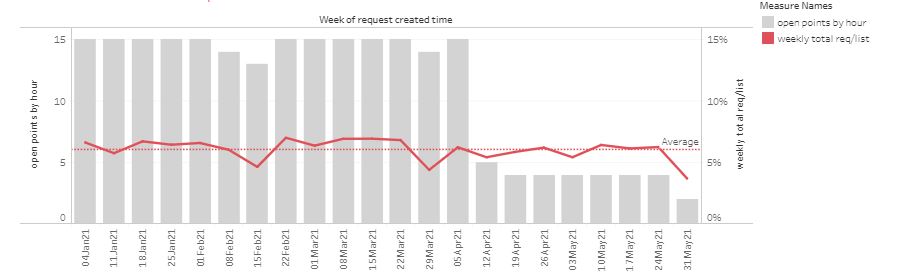
Another practice has made multiple changes in an attempt control demand, sometimes significantly reducing availability even in-hours.
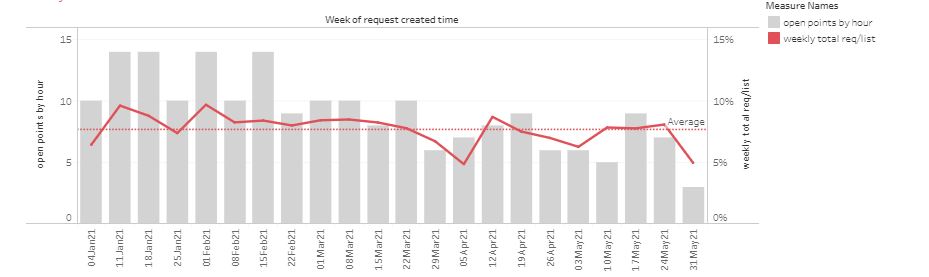 Overall, changing opening hours has had little effect on demand. However, as a patient there is a loss of service as they cannot be so sure they can submit a request online when they want to. Constantly changing the time the system is turned off risks patients losing trust in the online route, driving more demand through the telephone route which is less efficient to manage.
Overall, changing opening hours has had little effect on demand. However, as a patient there is a loss of service as they cannot be so sure they can submit a request online when they want to. Constantly changing the time the system is turned off risks patients losing trust in the online route, driving more demand through the telephone route which is less efficient to manage.
Taken to the limit, turning off online access completely would return to purely telephone access, with none of the flexibility for both patients and staff to use the efficiency of messaging and workflow.
Are there other advantages in cutting hours? Some take the view that they feel more in control if they know that no new requests can arrive after a certain time. Others turn off access at weekends, on the basis that some issues may have self limited by Monday, or they don’t want to see requests stored from the weekend, adding to a busy Monday.
Our usual advice to practices has been to keep online access open all the time, both in-hours and for OOH times when the message to patients sets a different expectation. However, we are clear that practices may turn off access themselves, either routinely or ad-hoc for example in the case of staff absence.
Based on the new data, we would suggest:
1. Reducing access hours has very little effect on total demand.
2. Practices may choose to limit hours, and it’s better to have consistent times so patients can be confident that online is open.
3. Whatever the decision, it should be up to the practice to determine access hours, and easily controlled by practice staff.
- Published in Evidence
Are you seeing higher than usual demand?
GP media is full of headlines to the effect that demand in general practice has been overwhelming in recent weeks. Our data from practices shows around 10% increase since January, peaking in March. Seasonal effects are normal, but is overlaid with the unpredictability of the pandemic (last year saw demand reduced 30%). There are real world reasons why demand is now high: secondary care waits, mental health issues and increased complexity. How can askmyGP practices adapt?
We don’t have a silver bullet but can offer some thoughts. Firstly, a couple to avoid:
– It may be tempting to delay non-urgent patients. This doesn’t really save work, as the patients still need to be dealt with and are more likely to chase, increasing stress.
– Shutting off online access when a number has been reached means patients will turn to the phone, increasing workload on the day, but they may lose trust in the online system longer term, increasing your workload.
We suggest continuing the tactics you would normally use, with these aims:
- respond rapidly to avoid patients chasing and rework
- encourage online access as it gives you the option to message patients
- manage the flow same day to keep you feeling in control.
1. Check the data that you have on demand, from your reports section. Trends over time will give you the longest view, while weekly demand shows the split by day of week. From the superuser menu Settings>Capacity planning helps with a simple way to estimate demand, as a % of your list size by week and by day. By default set to 6.5% of list per week for clinical and 1% admin, you can adjust these figures and save to dashboard. Some practices drive more demand eg repeat prescriptions through askmyGP, so it’s best to use your own figures.
2. Adjust rotas? Where possible, both timing and capacity (number of requests per session) will help. You’ll see on the dashboard how close total capacity comes to predicted demand, which is a good predictor of how well each day is going to work.
3. Adjust opening hours? Views differ on how best to organise. Many practices accept requests 24/7, responding only in core hours, and we’ve found that patients appreciate the convenience but rarely abuse the system. OOH requests are about 20% of the total, much of it just before opening time, and weekends are very low. Others don’t accept requests OOH or stop receiving requests some time in the afternoon.
Our evidence shows that this has very little effect on total demand (patients have to wait), but if the cutoff is too early, say before 4pm, it does drive demand onto phones which increases practice workload. Requests judged urgent should still be put onto askmyGP so the workflow is consistent and you have a true picture of total demand, while losing the ability to message patients.
4. Change service message? Any service message can be set at Settings>System to advise patients although we don’t know how well read they are. A short message is always better than a long one which is much more likely to be skimmed or ignored.
5. Assign new requests quickly especially at peak times. If there is likely to be a delay compared with normal service, you can send a preset message from the assign screen (“skip” bottom right, then the message dialogue appears)
They say that after rain comes the sunshine and we expect the normal pattern to be re-established before long. Roll on summertime!
- Published in Comment
What’s happening to GP demand?
Not for the first time in living memory, the GP media is full of headlines on demand taking practices to “breaking point”. It seems to me important that we bring the best data we can to bear on this question. It’s only good scientific discipline to diagnose the problem before attempting to apply a cure.
There are real world issues which could be driving some level of increased demand. Patients may have saved up issues during the pandemic for which now they want help. Long waiting lists for secondary care may increase the primary care burden. Concerns about covid, and long covid, may be part of the load. Complexity may have risen, with mental health issues more common. While all these are possible, I’ve seen no data to quantify the effects and we don’t know the detail of patient requests.
We can say that overall patient demand is at a new peak, compared with winter 2019 pre-pandemic, numbers up by around 5%. At this time of year demand usually flattens by a few % with spring weather so the relative change may be slightly higher. There is a much bigger change compared with April 2020, because demand fell by around 30% during the first lockdown.
How to measure?
While headlines can be made by choosing a suitable baseline, I think it’s vital to use consistent measures. Even though they are imperfect, the same measure year after year gives us a much clearer view than introducing different measures, imperfect in new ways. This is a key reason why we start from patient demand, driven by patients from outside the system it’s less subject to internal system changes.
How could system changes contribute to the headlines on demand? There’s public speculation that making access easier, particularly online access, could increase demand. No one can say that it’s never true, but pre-pandemic we found that overall clinical demand stayed predictable and constant around 6.5% of patient list per week, and was not affected by faster service. It is true that if supply was previously constrained then the true level of demand would become apparent, but this is not strictly new or increased demand.
English practices are being asked to provide new data, relating to appointments. Changing the measure to “activity” may seem a fine point, but if one patient request generates two activities (eg telephone call plus separate face to face) the activity appears to double, cf one pre-booked appointment. This could be misinterpreted as demand and on a large scale, very misleading numbers will follow.
So what to do?
There are calls to go back to the time before. I can understand that, at a human level we are acutely aware of loss of good times remembered. But thinking back, there were huge stresses, and patients who’d waited weeks to see the GP were suffering. Another form of double counting was the “just in case demand” – patients booking ahead speculatively, knowing that it’s hard to get an appointment.
Now there are calls to limit online access. We’ve always believed that practices should have control over their access channels, so they can programme times to accept new requests into askmyGP. The data shows that turning off out of hours has little effect on overall demand, and is only fair within the GMS contract, although we do have practices who accept requests at all times (and respond in hours).
However, if access is turned off too early, or after a fixed count is reached, unintended effects can follow. Once patients lose faith in the online channel being available, they return to the phone, taking up reception time in answering and more GP time as a phone call is needed in return, and the beauty of asynchronous messaging is lost. A downwards spiral results, where online demand falls, workload increases and waiting times increase, as does stress for all parties. Access becomes a lottery, and the very thing we want to avoid, digital inequity, returns. Those advocating the blunt instrument of limiting supply have not come up with a way to make it fair or based on clinical need.
Don’t give up!
Primary care has made huge and positive changes through the pandemic and we must not lose sight of the gains. I’m hearing of lengthening waits even for a phone call, queues of online forms awaiting triage, and many practices with very little incoming online or a token bolt on tool.
It has been striking to see askmyGP data show the proportion of requests resolved same day stay close to 83%, with half under four hours, even as demand has increased and face to face has ticked up to 10%. We’ve never said it’s easy, never said we’ve reached the destination, and our users are feeling the same real world pressures as all GPs. But I think we’re on the right track:
- online access for the large majority who can use it,
- digital triage in one click,
- a rapid, appropriate clinical response.
When times are hard, we can celebrate having in the UK one of the least worst primary care systems in the world. Given the ups and downs, let’s go forward rather than back.
“So much better service this is definitely the way forward thankyou.” Lincolnshire patient 8 minutes ago.
Harry Longman
- Published in Comment
Triage – do we need a new word?
We’re enjoying the sunshine, working a lot from home, and asking, how much has changed in primary care in a year, and how much hasn’t?
It seems quite a lot, as this sounds at face value rather like what we’ve been saying for ten years or so. NHS England planning guidance assumes that “total triage” should be embedded, and they mean permanently. Ah, but in the previous paragraph, they want 50 million more GP appointments! Well, that’s still based on supply led thinking, and I would so love to see a change of perspective, beginning with understanding demand.
Demand led thinking starts with the patient request, infinitely variable in every detail but conforming to quite predictable patterns both of timing and content. When access is constrained, it can be difficult to measure demand (because patients can’t get through), but trying to manage slots risks the wrong kind of supply and the wrong timing.
Unfortunately recent efforts to measure supply, requiring the generation of appointments, have served to exacerbate the problem by focussing minds on the numbers. “What gets rewarded, appears to get done. What gets punished, appears not to get done.” Human nature hasn’t changed, I think we can be pretty sure of that.
Yet the “total triage” tag has generated opposition, Helen Salisbury asking in BMJ “Triage is for emergencies. Can we start planning for a time when it’s no longer necessary?”
The origins of triage lie in war and emergency, from the French trier, to sort or select, and so “routine triage” may sound like an oxymoron. Before looking for a different word, it’s worth considering what is intended and what is the alternative.
The point of primary care is to cope with undifferentiated demand, and the NHS promise is for patients to have universal and free access. So long as they provide that access to their patients, GMS gives GPs full professional discretion as to how they do so. Reality bites because there will never come a time when there is sufficient capacity to give every patient exactly what they want, when they want, with whom they want and in the way they want.
As we’ve seen time after time, if patients have completely unlimited access to book a face to face consultation, while many use it well, some abuse it, but the problem is that you can’t know in advance who they are. More often, it’s not deliberate abuse but simply not knowing what’s needed, or from which clinician. Human nature again plays a part, scarcity ramping up demand. If it’s a long wait to get an appointment, I’d better book early “just in case”, and while medical need is unchanged, demand appears to rise.
That alternative reality inevitably means that patients must queue for as long as it takes, and we well remember the four, five and six week waits for appointments. I’m glad to say that particular noise has much abated this year, and however it is labelled, it’s thanks to GPs changing how they work. Still, it’s worrying to hear now of some patients waiting two weeks for a telephone call, which could still be called triage but is firmly based in a supply led system.
I suspect that much of the opposition to triage is that it is seen as a bolt-on rather than thinking and system change, which then means a gruelling experience of the process. Zoom fatigue, or telephone fatigue, is a reality. We need variety in the day, and we need human contact. Equally, wading through lengthy questionnaire forms is tiring on the brain both for patient and GP, where with too much information the first task is to sort the wheat from the chaff.
Returning to the goal of the system, we want to meet the patient’s need, in the most efficient way for the GP. Starting the process online is the best way we know for the vast majority of people, as in other spheres of life. We’ve found trusting the patients to use their own words in askmyGP has three key advantages:
– it’s simple and the computer never says no, so typically 70 – 80% of all patients will use it online.
– it’s fast to assign to the right clinician
– the GP has sufficient information to know the best approach, even if that needs a change later on. Time is only committed appropriate to need.
It’s never easy to change language and I don’t know whether “sort” is an improvement on “triage”, which at least has a medical association. Perhaps we should settle for describing the alternative as “unsorted”. I don’t think anyone wants to return to the waste of precious time seeing the wrong patients while the right patients were hanging on the phone trying to get through. GPs tell me a year since making the change, it came at exactly the right time and we’re never going back.
Harry Longman
Photo: Otis Historical Archives Nat’l Museum of Health & Medicine
- Published in Comment
Remote GP care and inequality – dispelling the myths
Calls for a review into how patients access their GP, and the potential barriers to them doing so, have highlighted the difficult decisions some practices are facing over remote consultations. The focus on video consultations, as opposed to remote or total triage systems, is based on concerns about equity.
Healthwatch England called for the formal review after its new report revealed the rapid switch from face to face to remote consultations in the last year has not met everyone’s needs. It found some patients are struggling to get through to their GP surgery, while other concerns include possible missed diagnoses, difficulties for people who don’t have access to the internet and for anyone whose first language isn’t English.
The NHS Long Term Plan stipulated that remote consultations (telephone or video) should be offered to all patients by 2021 but early take up was slow and the Covid-19 pandemic has been the catalyst for change. However the sudden necessity for remote consultation has revealed much about the preferences of many patients.
While an RCGP survey in July 2020, reported that more than 88% of UK practices were now equipped for online or video consultations compared with just 5% pre-pandemic, a King’s Fund report into digital access to GPs during the pandemic highlighted research which found that some of the initial enthusiasm for online access is beginning to wane.
Providing choice over method of consultation is vital
To ensure that gains made during the pandemic with regard to remote consultations are not gradually eroded, patients must be able to access services in a variety of ways. Making sure patients have access to online or video consultations is just the start.
Choice about the type of consultation and the ability to provide remote access to a GP (whether online or by telephone) is key. The Healthwatch England report found that, out of 1,190 people polled who had booked an appointment since March 2020, 75% had booked via telephone, 18% over the internet and 5% in person.
All too often video consultations are seen as a proxy for remote access to a GP, but not everyone wants or is comfortable with this way of communicating. However, there are several different online systems that can provide options to suit the patient. For instance, askmyGP provides a unique total triage platform for patients to access their GP in whichever way they choose. Offering an online booking service to those who are comfortable using it can relieve the pressure on phone lines, particularly at peak times.
We regularly review data from our system which is used by over 2 million patients to access their GP practice. This data tells us that several myths about remote access simply do not stand up to inspection. Here are just a few we have looked at:
“Patients prefer face-to-face consultations”
A typical GP practice sees about 5-8% of its list size each week and askmyGP is often handling that entire volume. 73% are going online to make requests and 27% are phoning the practice. With more people going online to make an appointment request, this relieves pressure on the phone lines for those who prefer to call. For our GP practices only 6% of patients requested a face-to-face consultation which shows that patients are happy to go online or use the telephone to access their GP.
“Older people are not internet savvy”
Older people make up a significant cohort of the patients using askmyGP to access their practice, still 50% at 70-75. However, for anyone less confident in using online services or who cannot access them, our triaging system ensures choice. Patients can still call the surgery and the receptionist can key in their information and arrange their appointment instead, it doesn’t have to be all or nothing.
“Remote access is unsafe”
Using askmyGP, practices can respond to requests appropriate to the patient need, rather than limited by supply slots. The BMA has also highlighted that the speed and convenience of access to GP services has improved for many as a result.
So, it is clear from our data that patients are happy with remote access, mostly by telephone or message, but providing choice over how appointments are accessed is key. An efficient triaging system can provide that choice and ensure that everyone is able to access the services in the way that is the best and safest for them.
Click here for more on how we can help.
- Published in Comment