askmyGP joins Evergreen Life for a huge step forward in patient-led healthcare
Evergreen Life is proud to announce the acquisition of Salvie Ltd, the creators of online consultation and workflow system, askmyGP. The two will now work together to help GPs, Clinical Commissioning Groups, Primary Care Networks, and health boards to manage caseloads and strengthen relationships with patients.
The acquisition presents a valuable opportunity for both companies to harness the others’ technical expertise and software experience. The two combined will allow for a wider scope of operations in primary care and better patient engagement, helping both companies progress towards their shared vision of facilitating better access to healthcare for individuals.
What is askmyGP?
askmyGP allows patients and carers to outline their issue quickly and simply in their own words. This enables busy surgery teams to efficiently triage requests, prioritise patients appropriately and minimise wait times. Founded by Harry Longman, askmyGP has been supporting GPs in managing their workload since 2011.
askmyGP serves GP practices with over two million patients and now expands Evergreen Life’s primary care services to include online consultations, including secure video and messaging. Individuals can be assured they always receive medical advice from trained NHS professionals via easily accessible digital channels, further developing the trust between patient and clinician.
What is Evergreen Life?
Established in 2014 in Manchester by former clinical pharmacist, Stephen Critchlow, the Evergreen Life app provides a handy way for people to access their medical records electronically and manage their healthcare online – users can request help or order a repeat prescription. The app also offers Wellness Check functionality to help people better understand their health by taking clinically-reviewed questionnaires to improve various aspects of their wellbeing such as sleep, fitness, diet and happiness.
“We believe in putting the individual at the heart of their own healthcare, so people can be empowered to get the health and wellbeing they want and get access to support when they need it. askmyGP is leading the way in person-centred solutions by making it easier for patients to talk to their own doctor and help GPs to prioritise and deliver care through message, phone and video. By working together and through the new Evergreen Connect platform, we can join up more areas of the health and care system as part of our mission to deliver People Powered Health,” said Mark Hindle, COO of Evergreen Life.
“We are joining a company well-established in the healthcare technology industry and which complements our work in being able to offer more to patients, GPs and other healthcare providers. askmyGP enables over 200 GP practices around the UK to manage their workflow and respond to patient demand with outstanding service, resolving 79% of requests on the same day,” said Harry Longman, CEO and founder of askmyGP.
Patients will benefit from a wider range of services and communications with their GP, and through the Evergreen Life app will be able to take better control of their own health. Providers will benefit initially from integration with clinical systems across the full range of patient facing services and better communications with patients through the app. As our products and services develop, they also gain from people taking control of their health, wellbeing and medical records.”
For more information about Evergreen Life visit: https://www.evergreen-life.co.uk/
ENDS
- Published in News
GPAD data submissions to NHS England
This note is to update users on data submissions to NHS England for activity reporting.
You may know that practices are required to submit activity data from 30 June 2021 as outlined on their website here.
Many practices made representations that this would create extra work for no benefit, as many patient requests are completed with no need for an “appointment” record.
We have seen a copy of a post on the forum “FutureNHS” by “Digital First Primary Care”
We are raising this with system suppliers with the aim to gather that data directly from them. If a Practice has started / or is happy to map across both systems, this would ultimately create a better reporting data and Practices can continue to do this.
However, if this is not currently being recorded in the GP Clinical system appointment book, the current advice is not to double record in the GP Clinical System appointment book due to the extra burden on Practices.
When the data is published it will include a caveat highlighting that the GP appointment book is not the only tool which captures appointments and for those appointments captured elsewhere we have not got the means of capturing that data.
We have requested an official communication to this effect but have had no reply so far.
The message seems to be a positive one, there is no need to double enter and no further action is required.
We have enabled a feature in askmyGP which allows you to specify a role, compatible with GPAD reporting, for each staff member. We suggest you state a suitable role from the drop down list in the staff record, which is done only once and would take a few minutes for the whole practice. Any reporting needs should then automatically be covered.
- Published in News
General Practice Appointment Data – reporting to NHS England
In order to help you meet your GPAD obligations, and improve reporting in the practice, staff ‘profession’ needs to be recorded consistently. This note explains the process, context and wider benefits.
English Practices have recently been asked to provide appointment data via their CCGs to NHS England. As you will know, we believe that a flexible triaged approach supports practices to utilise their time to best effect for themselves and their patients. This view appears to be reflected in NHS England’s guidance on ‘total triage’.
We remain in discussion with NHS England, because we feel that you are being asked to report data that may not accurately reflect the activities carried out in the practice. In addition, we have made some changes to resolve the immediate issue, which is to minimise the administrative burden for you in completing the reports.
To enable a report to be produced, consistent descriptions of ‘profession’ are needed to meet the GPAD requirements. Pragmatically, this means that all staff professions need to match one of the exact descriptions recognised by NHS England. The new ‘Professional Group’ list allows you to select the best match for each staff member. This is accessed via Staff > Edit, or Settings > My Profile. There is a short note available: https://askmygp.zendesk.com/hc/en-gb/articles/360006981297
Although this work is in response to GPAD, there are some more general benefits. By using consistent descriptions of profession, we will be able to provide you with better reporting in relation to staff groups – for instance allowing capacity planning by profession, or better understanding the activity of groups within the practice.
As always, the quality of any reports produced are dependent on the quality of the input data. Obvious limitations of reports from askmyGP, besides data quality include:
- any activity not recorded via askmyGP will not be included e.g. Nursing or Clinic activity booked directly.
- We cannot report on data (such as profession) which has not been entered into the system.
- GPAD guidance permits some contacts to be counted twice. We will try to ensure that we include this, however it may not capture a small percentage of this double activity contact.
We will add a report to your system in the near future. Should you wish us to provide reports directly to your CCG please contact us via your Training Partner to discuss details.
- Published in News
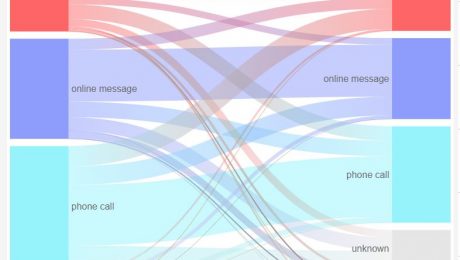
Announcing askmyGP live analytics
Britain is social distantly dancing in the street, singing to the screen and rediscovering family games behind closed doors.
Here, working away from askmyGP Towers, the nerd unit has been in hyperdrive (we’re all a bit nerdy) and we are delighted to present, drumroll,
Yes indeed, all the data from 2 million episodes, aggregated and anonymised, is in the public domain for anyone and everyone to crawl over.
- What proportion of demand arrived at all our practices last week online? 74%
- Median completion time for all patient requests last week? 87 minutes, 52% faster than three weeks previously
- Proportion of requests completed same day? 91%, up from 81% three weeks earlier
- How many patients requested a message response?
- How much has face to face dropped?
- How has patient satisfaction changed?
I’ve left some for you to explore and there’s much more.
The overall message is: access is better than ever, though very few are seeing the GP face to face. And patients are mostly very happy with that.
It’s been a full on week for us with new practice launches every day now. Delightful stories come up all the time, such as Mai, PM at Ingham, Lincs, quite moved as she explained “Tuesday was non-stop on the phones, then Wednesday we were online and suddenly, quiet like I’ve never seen in all my years here.”
A string of health boards, CCGs and PCNs have now asked us to launch all their practices double quick, across parts of South Wales, South West, Greater Manchester and Lincs. Trafford CCG is a great example, one of their practices St John’s Altrincham on our new video.
We too are being forced to unlearn and remodel how we deliver, it’s exciting!
Have a great weekend and not too much screen time.
Regards
Harry Longman
PS We decided not to be one of the 11 suppliers in the NHS England DPS online/video offer randomly allocated to CCGs. However, we were told at the NHS England webinar on Weds that there’s a “Single Tender Waiver” procurement route which CCGs can take, no idea of the details yet but let me know if you are interested.
- Published in News
Our response to DHSC Code of Conduct
The Department of Health and Social Care published on 19/2/2019 its Code of Conduct for data-driven health and care technology.
Our response to the ten principles follows:
- Understand users, their needs and the context. askmyGP users are broadly two groups, patients and providers which includes all GP practice staff. Our design principles are for simplicity and ease of use, a difficult task when appealing to patients of all ages and abilities, both in general education and familiarity with online tools. We cater equally for proxies (parents and carers), all gender expressions, and keep language simple to help those with limited English. To assess our effectiveness we monitor age specific adoption by patients in each practice, and feedback from patients informs our development process.
- Define the outcome and how the technology will contribute to it. Our mission is to make it easier for patients to get help from their own GP, and easier for GPs to provide that help. We measure attainment against this outcome by volumes, response and completion times, and measures of efficiency through resolution mode by providers. We also collect and monitor patient feedback and present all measures to the provider organisations.
- Use data that is in line with appropriate guidelines for the purpose for which it is being used. We comply with all relevant legislation including GDPR, Data Protection Act 2018 and collect data only for necessary purposes. Personal data is processed on behalf of providers (the data controllers), stored and transmitted encrypted and over the secure N3/HSCN network. Anonymous data may be used for research and marketing purposes as allowed under the same principles.
- Be fair, transparent and accountable about what data is being used. All data is used in accordance with Caldicott principles, and the conditions are agreed by patients and providers.
- Make use of open standards. We support the use of open standards and wherever technically possible provide open links to others for legitimate interoperability reasons. We use standard NHS number coding for any authorised data transfers.
- Be transparent about the limitations of the data used and algorithms deployed. We collect and transmit plain text and other file formats between patients and providers, but we do not use algorithms to produce triage decisions or advice to patients.
- Show what type of algorithm is being developed or deployed, the ethical examination of how the data is used, how its performance will be validated and how it will be integrated into health and care provision. We do not develop algorithms. We do offer a third party service with Isabel Healthcare, which uses a machine learning approach. Our users may enter any number of symptoms, and be shown a range of possible conditions.
- Generate evidence of effectiveness for the intended use and value for money. Integral to our offer to all customers is standard reporting on usage, patient service, timeliness and efficiency through the use of askmyGP. We provide an economic model (Loadmaster), configurable by each customer, which demonstrates their value for money. We also conduct our own analysis of performance and value and may publish on this site and in other media from time to time.
- Make security integral to the design. From the outset of design, security has been built into askmyGP. Key features include:
- N3/HSCN access required for all live patient data by providers.
- Encryption of all patient data in transit and at rest
- Strength checked passwords required for all users.
- Separate code and database for live and demo systems
- Independent penetration testing and fulfillment of all comments raised.
- Define the commercial strategy. Our strategy is that self-funding customers should see a high rate of return from their investment, and do so from the date of launch (typically four weeks from engagement). Growth is therefore not dependent on taxpayer funding, but on efficiency and financial savings generated through the use of our services.
Harry Longman, 21 February 2019
- Published in News
askmyGP launches video consulting
We’re delighted to have reached a milestone today, just over four months after launching version 3. Steve Black our chief analyst told us:
“At 08:31 this morning Aisha at Balaam Street closed the 100,000th patient episode.”
Wonderful to know that in the absence of a functioning government, some things keep rolling along.
History is informative but I’m even more excited about the present, as we announce today the launch of video consulting through our askmyGP platform.
- No app to download
- No need to change surgeries
- Works on any device with a camera
- Your own NHS GP initiates the call
The first ones have happened already, one GP telling me of a child he could see happily running around- saving a visit, and a mole he could tell was benign – giving reassurance. Another tells me of checking on a wound and saving a whole morning off work for a patient.
The experience was easy for both parties, with high quality pictures over wi-fi, and no cumbersome pre-booking arrangements.
Video consults are driven by what is clinically appropriate in the GP’s view, and it’s going to be so interesting to see how this mode affects practice. My guess is it will be around 5 – 10% of consults, but this is the thing: we don’t know.
Have a lovely evening.
Regards
Harry Longman
![]()
- Published in News
Enjoy the summer?
Looking out on the rain, memories quickly fade of, for once, that glorious bank holiday weekend.
In GP land you may have noticed a lighter week too, because demand is predictably sensitive to weather – whether warm sunshine or heavy snow.
We need to qualify the effect however, because if your system is book ahead and wait, lower demand only shows up as a smaller backlog and maybe less pressure on reception. You will still see the same number of patients who have patiently waited whatever the urgency of their need, and it will feel like a treadmill.
The point of a demand-flow system is that there’s always plenty of capacity for the predicted demand, and if it comes in below prediction, you can enjoy the sunshine. A colleague of mine visited one practice we work with on Thursday lunchtime and there were just no patients, time for chat.
Now with summer on the way it is of course the perfect time to put that demand-flow system in place but let me tell you about a real problem we are struggling with.
I can name three practices right now where they are very clear on the challenges they face, they can’t cope with the workload, they know the service is terrible, and their receptionists are getting abuse every single day.
They’ve done a thorough analysis, all the surveys, know exactly what to do, and four GP partners can hardly wait to get going. But one, or perhaps two, partners have dug their heels in.
I’m a great fan of the partner model for a host of reasons, and I haven’t seen a better one, but it has its drawbacks. One partner can veto any change. They are condemning the others to live with the same or worsening situation. Why isn’t there a veto on doing nothing?
Fundamentally I think this imbalance in favour of inaction is holding GPs back, perhaps the whole profession, even if a majority can see what needs to be done.
Are you in this situation or do you have any suggestions?
Meanwhile two north east practices launch on Monday and let’s hope they enjoy the summer.
Kind regards
Harry Longman
PS: One who did act was Dr Sue Arnott and she joins us for this Thursday’s webinar at 1pm.
Online consultations – what is working and why?
Some background on how she came to be running a 4,700 practice as a single hander here.
Many have asked for the first in the series recorded, so it’s here, 45 minutes, “Exploding the myths of online consultations”
- Published in News
Revealed: the tiny take up of NHS111 digital and its alarming dispositions
NHS England has trialled four digital versions of NHS111 in an attempt to shift channel from telephone to online.
An internal report dated December 2017 and obtained through HSJ reveals the astonishingly low take up of these heavily marketed pilots. Download the full report here:
Data contained within the report shows the four trials covered a population of 7.5m for the period February to June 2017. The total completed digital triages came to 8671.
A separate chart shows NHS111 telephone volume at around 1 million per month, for a population of 50m.
The digital trials covered around 15% of the population, and over the 5 months of the trial would see pro rata around (15% x 1,000,000 x 5 months) = 750,000 calls.
Digital triages therefore accounted for 8671/750,000 = 1.2%
We know that the digital option was heavily marketed in the four pilot areas, in the public domain, GP surgeries and through IVR messages. We have no idea of the costs incurred.
We can see by comparing the charts that conversions from “I registered or downloaded the digital solution” to “I completed a triage” range from about 60% for Babylon and Sensely to 30% for Pathways and 10% for Expert 24.
Figures given on dispositions are compared to 111 phone triage dispositions and what is striking is the similarity. Much is made of the 18% advised to self-care. However, it is very disturbing to see 20% advised to call 999 or go to emergency. Compared with GP audits of their demand, which they rate at around 0.5% as emergency, these are astonishing numbers. Work we have analysed with a GP led OOH service showed GP disposition to ambulance at 1.4%.
Following the advice of the algorithms would multiply use of emergency services by a factor of 10 to 20.
Worse than this, we suspect that the low take up means the diseases entered are highly unrepresentative of the overal disease burden, and are likely skewed to conditions which are “easy to triage” and therefore less acute.
Given the above analyses, and if you knew the eye-watering costs incurred, what would you do?
Harry Longman
PS The conclusion of the report’s author may surprise you, page 4:
The learning from these pilots supplemented with data from other health systems and from
other online services would continue to support the case for an online interface for urgent
care. This evaluation does not recommend one product over another but demonstrates that all
products have some similarities and differences but all products tend to support channel shift
and management of demand whilst providing patients with a good experience.
To gain further understanding of NHS111 Online and the impact on the health system, larger
data sets and linked data will need to be considered. Therefore, the expansion of pilots and
further analysis will enable a more robust evaluation.
- Published in News
One small Scottish practice changing the world
When there’s a chink of light in the dead of winter (and wall to wall NHS crisis on the BBC) we have something to celebrate.
I spoke with Dr Sue Arnott, who runs a practice of 4,600 patients in a traditional ex-mining community in central Scotland. She had tried for months and failed to recruit a GP, so is now running single handed, supported by an ANP and further part time nurses.
She explained how they are now up to about 60% of demand online, of which she responds by secure message to about 60%, largely without even a phone call. It means she has time for all the patients’ needs, in the appropriate mode, today, and is on top of demand, feeling in control.
How? There’s no coercion involved, just that the receptionists point the patients to the website, show them where to start and help as needed. If not possible, they’ll take the request by phone. And patients are very very happy.
When we were first in touch in the autumn I was more than a little concerned about the few GP sessions for the list size, and said they’d need to go all out for change. They have, they love it and they are providing a fabulous service. That’s my cause for celebration, because anyone can do it.
Philip Hammond is not going to bung any more money into the NHS. Even if he did, Jeremy Hunt is not going to magic 5,000 GPs out of thin air. (and I submit that it’s immoral to recruit them from nations where doctors are even scarcer).
Patient demand is not going to go away because we tell them to self-care more (we’ve been telling them for decades. They know).
So we have the demand that we have, and the GPs that we have. But by changing the system in every practice in the UK, which is up to every GP in the UK, we can manage.
Indeed we can thrive, like one practice in Lanarkshire.
Harry Longman
- Published in News
PRESS RELEASE: askmyGP overcomes NHS Choices search gremlins
PRESS RELEASE 3 January 2018:
askmyGP overcomes NHS Choices search gremlins with new free webapp
——————————————————-
Patients are being urged more than ever to self-care, in order to cut demand on NHS GPs in the winter season. While NHS Choices provides high quality advice, until now searching the site has been hit and miss.
askmyGP, the leading online consultation platform, announces today a free version which lets patients search NHS Choices with a unique smart search algorithm.
Founder Harry Longman explains the reasoning:
“We’ve always directed patients to seek self-care advice from NHS Choices. It covers virtually every medical condition, the information is clearly presented, evidence based, and free. It carries no advertising and never tries to sell to patients, whether medications or consultations, as other sites do.”
But the weak area has been search. Put “Back of knee hurting” into NHS Choices and you’ll see “La Bomba dance workout video” – not exactly what you were hoping for.
The same phrase entered into askmyGP takes you straight to knee pain and its potential causes.
Many similar examples are exactly as entered by real patients. “3yr old holds his breath”, NHS Choices: Your guide to an echocardiogram. Or Dentures. Perhaps not.
“Had coff for over 5 weeks”, gets you Norman’s Hip Op video.
Try all these in the askmyGP demo site and compare with NHS Choices itself, even though all our content is provided by NHS Choices. What patients want is a smart but sympathetic search which won’t quibble over how they spell diarrhoea (we’ve found the right page with hundreds of spellings in askmyGP, from diria to dhearrorrea).
We don’t believe NHS Choices content should be reformatted and sold back to the NHS for private profit, as some suppliers have done. What we sell is the askmyGP online consultation system, helping more GPs and patients every week (over 25,000 episodes managed so far).
We’re giving away the very best we can offer to help patients self-care. The askmyGP search webapp is available from January 2018 to all NHS practices and organisations, no strings attached, it’s free, for everyone and for anything.
ENDS
Note to editors: askmyGP is provided by GP Access Ltd, founded in 2011 with the vision “To transform access to medical care.” We are serving NHS GP practices, CCGs and Health Boards in all four countries of the UK.
Further information:
askmygp.uk Search demonstration at Bramley Demo Surgery bramley.gpsurgery.net
Chief Executive Harry Longman, 01509 816293, mobile 07939 148618
- Published in News
- 1
- 2